E-Prescription App Development: A Comprehensive Guide


In recent years, digitalization in fields such as healthcare has reached an unprecedented scale. And that’s a positive shift! In many institutions, systems used to be so rigid and approval chains so long, that implementing new technologies would take years. Now, medical facilities have a clear understanding, that their systems need to evolve in line with market demands.
Luckily, prescriptions are one of the clearest examples of the positive shift. For decades, handwritten scripts have been a routine part of clinical practice. But, they have also remained a constant source of errors! We saw it all ourselves – from illegible handwriting to lost info and delays in processing. In an environment, where even minor inaccuracies here can put patient’s health in literal danger, there is no place for such errors anymore. That’s why e-prescription systems emerged. It is a right response to the need for greater accuracy, transparency and proper control in the prescribing process. So, in this article, we will take a closer look at e-prescription app development from a practical perspective. We will explore:
- trends shaping the e prescription app development market
- core system architecture and features
- common mistakes teams make when building such apps and how to avoid them
- compliance with guidelines and more!
The Role Of E-Prescription Software in 2026
The evolution of e-prescription apps reflects a broader transformation of healthcare systems. They evolved from fragmented paper-based processes to interconnected digital ecosystems with constant data flow between stakeholders. Here, one consistent pattern becomes evident. The primary driver behind the so-called eRx adoption is not convenience. It’s the need to address deeply rooted issues such as medication errors, prescription abandonment, ineffective slow coordination between providers, pharmacies and insurers.
Another defining trend is the shift toward interoperability. Modern e-prescription apps are no longer built as isolated systems. They have become components within a larger digital health ecosystem, tightly integrated with:
- electronic health records
- pharmacy management systems
- insurance databases.
This allows doctors to access all patient data in real time. Thus, patient prescriptions can be processed, validated and fulfilled much faster.
At the same time, the rapid expansion of telemedicine, especially after Covid pandemic, has reinforced the role of e-prescription systems as a natural extension of remote care. Now, clinicians are able to complete the full treatment cycle, from consultation to medication delivery, within a single digital workflow.
Equally important is the growing reliance on clinical decision support systems. Basically, they transform eRx platforms from passive transmission tools into active participants in the treatment process. As these systems get the access to patient history and potential drug interactions, they can directly contribute to a smarter treatment plan.
Who Are E-Prescription App Users?
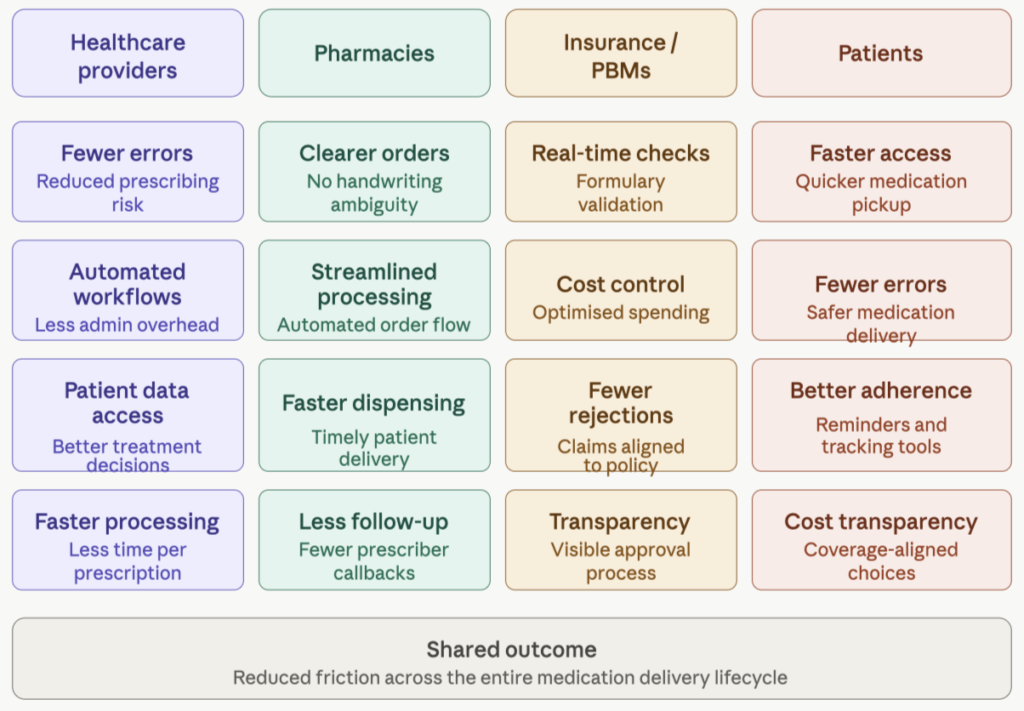
E-prescription systems operate at the intersection of multiple stakeholders:
- healthcare providers, hospitals, clinics, individual practitioners,
- pharmacies
- insurance providers and pharmacy benefit managers
The app serves different purposes for each party. For patients, although they are not the primary users of eRx platforms, the benefits are also tangible.
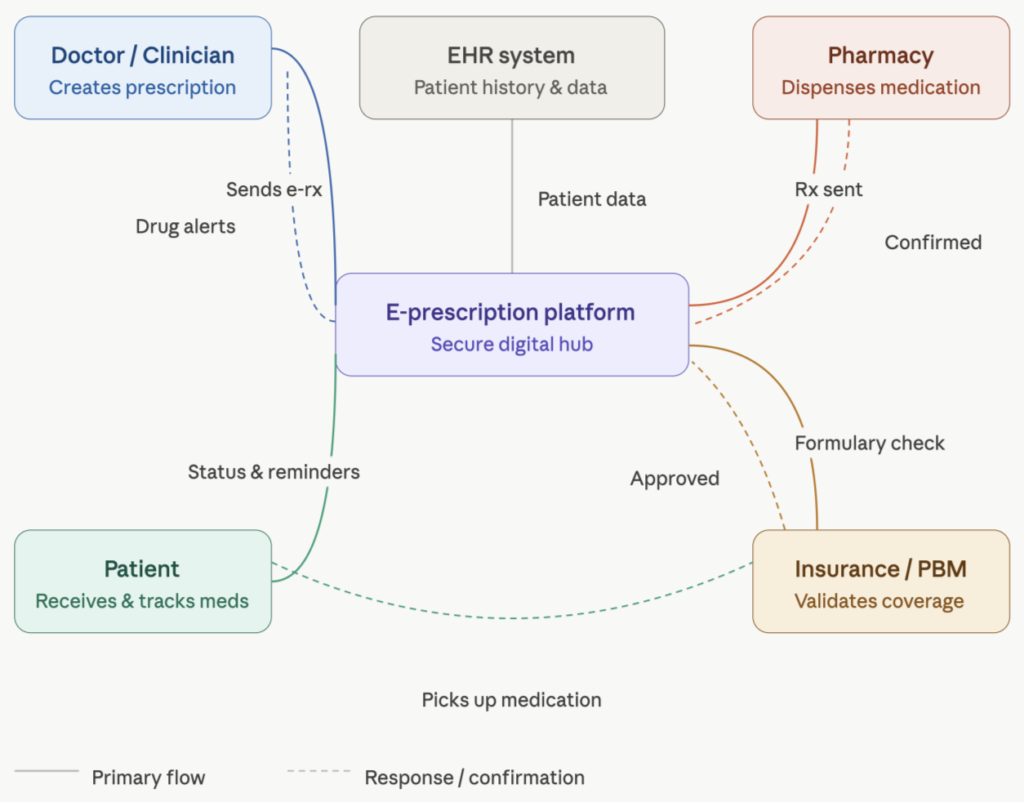
Must-Have Features of E-Prescription Apps
From a structural perspective, an e-prescription app cannot be reduced to a single interface or standalone product. Its functionality depends on continuous interaction with multiple external systems. At its core, such a platform acts as a data integration hub. It connects electronic health records, pharmacy networks, insurance databases, regulatory monitoring systems. This unified workflow makes all relevant info, from drug availability to insurance coverage, accessible at any moment. Another essential element is the integration of insurance and formulary data. It allows clinicians to assess possible financial implications. For example, if a patient’s coverage is not enough to get an expensive option, the system could suggest alternative i.e. more affordable medications.
The prescription management functionality – creation, validation, transmission, and renewal of prescriptions, must be executed seamlessly to maintain workflow continuity. When it comes to the feature set, it’s pretty standard:
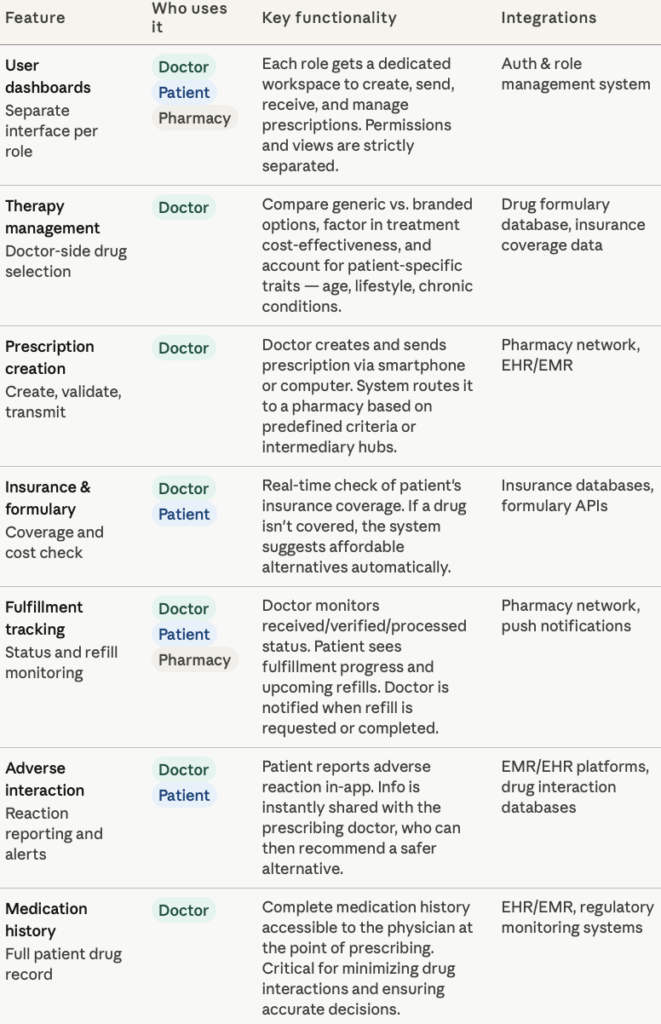
User Dashboards (Separate One For Each Involved Party)
Separate interfaces for different user groups: prescribers, patients, pharmacies, other stakeholders. Each role must have a dedicated dashboard to create/send/receive/manage prescriptions.
Therapy Management (Doctor Side)
The system should allow physicians (or prescribers in our case) to compare and select from equivalent medications and alternatives including both generic and branded drugs. It is also important to factor in treatment cost-effectiveness, along with patient-specific characteristics – age, lifestyle, existing chronic conditions.
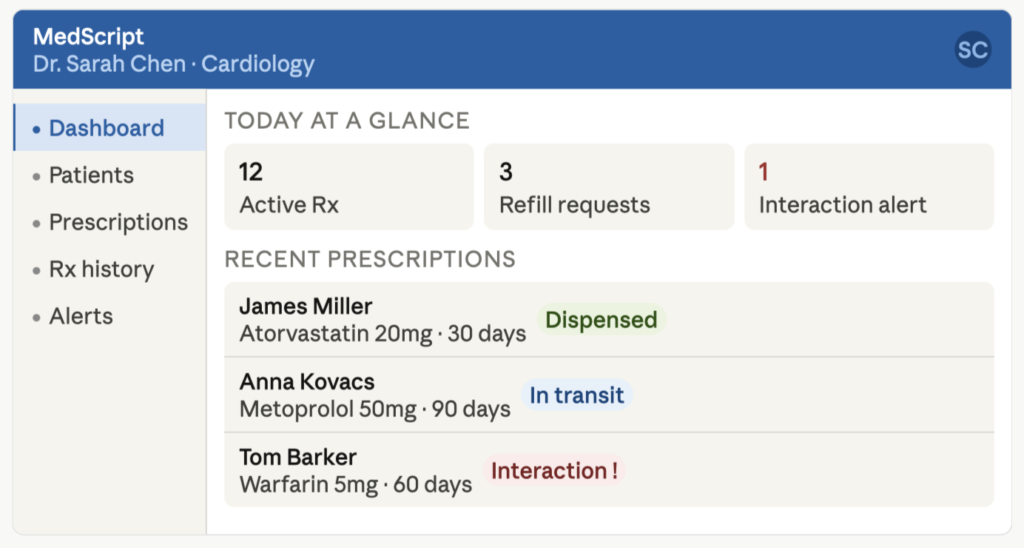
Prescription Creation and Submission
Doctors create new prescriptions and send them to patients via smartphones or computers. Once a prescription is issued, it is typically routed to a pharmacy, based on predefined criteria. Although, additional routing options, such as intermediary processing hubs, can also be offered.
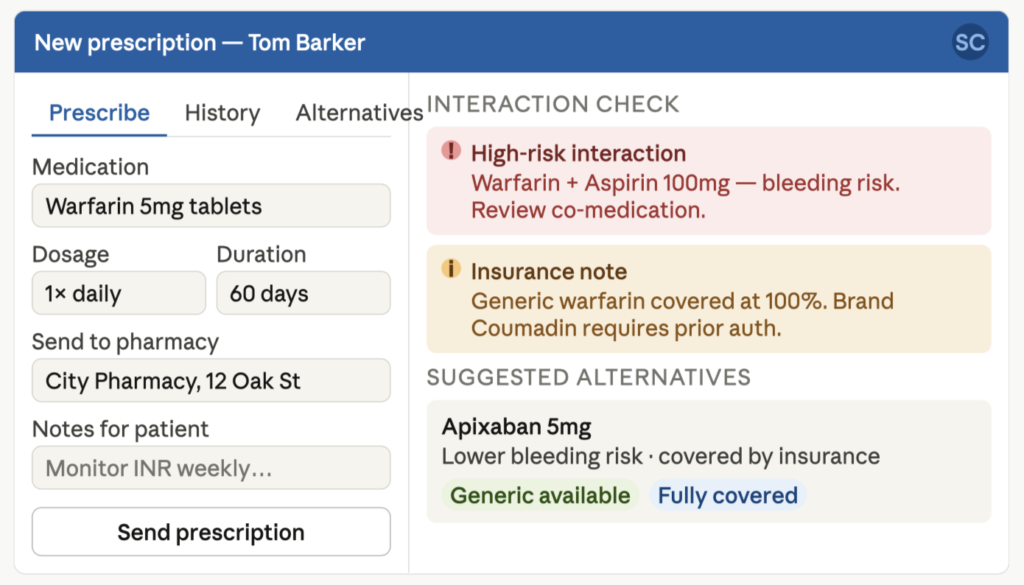
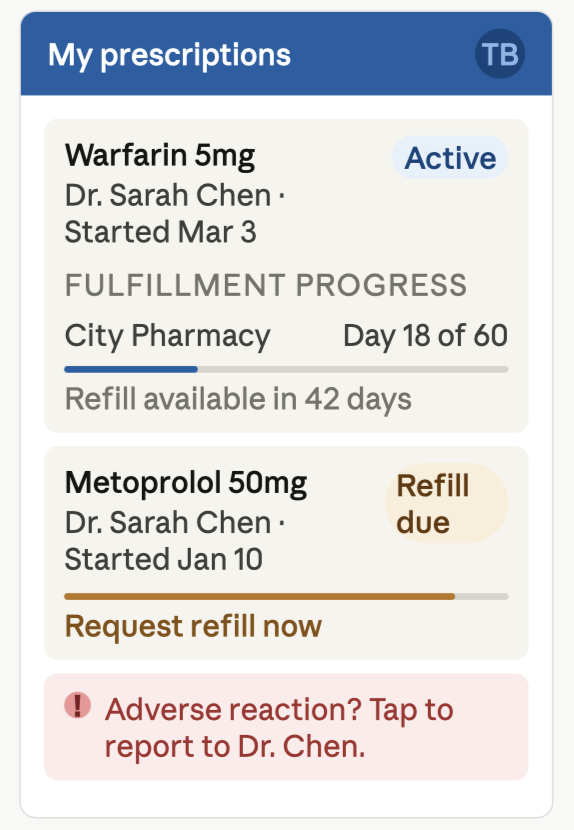
Prescription Fulfillment Tracking
After a prescription is sent to a pharmacy, physicians monitor whether it has been received, verified, processed. Patients should also be able to view the status of their prescriptions. This includes fulfillment progress and upcoming refills. In turn, doctors should be notified when patients request or complete refills.
Adverse Interaction Monitoring
If a patient experiences an adverse reaction, they should be able to report it within the app. This info is shared with the prescribing physician. They can recommend safer alternatives in this case. Implementing it is most effective when the system integrates with EMR or EHR platforms.
Medication History Access
Physicians should get access to a patient’s complete medication history. Critical for ensuring accurate prescribing decisions and minimizing drug interactions.
Step-by-Step Development of an E-Prescription Application
Before thinking about features or technology, focus on how prescriptions are actually created and used in the clinic. How does a doctor:
- access patient history?
- choose medications?
- communicate with pharmacies?
At this stage, the goal is simple: map out the exact journey from diagnosis to medication pickup.
Define the Core Functionality
An e-prescription app doesn’t need to do everything at once. In fact, trying to build a “full platform” from day 1 will lead to unnecessary complexity. Your goal is a strong MVP at the start, where a strong starting point includes:
- secure doctor login
- patient selection
- prescription creation
- basic validation (dosage, format)
- sending prescriptions to a pharmacy
Everything else—analytics, AI suggestions, integrations—can come later. Concentrate on the basics.
Design for Clarity, Not Just Features
This is where many projects fail. As we said above, if the interface is confusing, doctors may enter incorrect info about the medication/dosage. Pharmacies, in turn, will misinterpret what was sent. It can directly affect patient safety. Thus, your priority is to:
- minimize manual input
- use structured fields instead of free text
- provide clear, readable prescription formats
- reduce the number of steps required to complete a task
Compliance from Day One
Healthcare software operates in a highly regulated environment. Depending on your region, you may need to comply with:
- data protection laws (like GDPR)
- healthcare-specific standards
- electronic signature requirements
Trying to “add compliance later” is one of the most expensive mistakes you can make!!!! It’s far more efficient to design the system with these constraints in mind from the start.
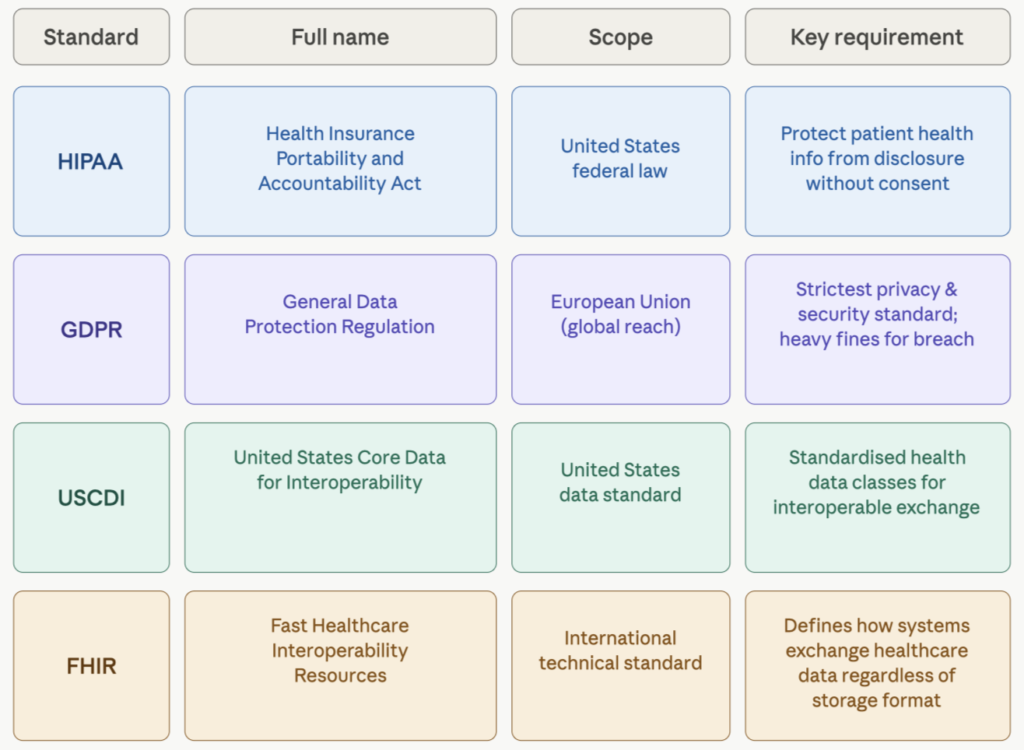
Integrate with Existing Systems
Most clinics already use some form of electronic health records (EHR). Your e-prescription app should work alongside them. This means connecting the app to:
- patient history database
- medication records
- allergy info
- other systems the clinic actively uses and relies on.
Build a Reliable Pharmacy Connection
An e-prescription is only useful if it reaches the pharmacy correctly. Depending on your market, this may involve:
- direct integration with pharmacy systems
- working with national prescription networks
- or using intermediary platforms
The key requirement is reliability, prescriptions must be delivered accurately, without delays.
Test in Real Conditions
In the best case, you will also need a real focus group of doctors to validate all aspects. Also consider pilot programs with real clinics before a full app rollout. You need to validate:
- how doctors actually use the system under time pressure
- whether prescriptions are interpreted correctly by pharmacies
- how the system handles edge cases.
Launch Gradually. Improve Continuously
A successful launch is rarely a “big bang.” Instead, most teams:
- start with a limited rollout
- gather feedback from doctors and staff
- refine workflows and usability
- expand gradually
E-prescription systems evolve over time especially as regulations and clinical practices change.
Common Mistakes in E-Prescription Development
One of the most significant errors is treating the system as a standalone app. In reality it cannot be disconnected from the network of clinical/operational systems. Without deep integration into electronic health records, pharmacy infrastructures, insurance platforms, the app cannot access the data, necessary for the decision support. Otherwise, we reduce its functionality to basic prescription transmission.
Another common pitfall is the underestimation of regulatory complexity. In this domain, legal and ethical rules are obligatory to follow. We talked about them above in this article.
Similarly, some developers focus on implementing surface-level features, while neglecting the depth and accuracy of clinical decision support. It results in systems that lack the intelligence needed to provide value to doctors.
User experience design represents another critical area where mistakes occur. In consumer apps, poor usability only affects engagement. In healthcare, it may have direct implications for patient safety! It’s very easy to explain. If the functionality is unclear, doctors may enter incorrect info about the medication or its dosage. In turn, the pharmacy may also misinterpret the received data. As a result, the patient may receive the wrong dosage or even the wrong medication altogether!! Plus, very complex interfaces can even discourage adoption among practitioners.
Final Thoughts
At its core, an e-prescription app is not just a digital tool. It fact, it becomes part of the clinical decision-making process! The most effective solutions are not the ones packed with the most features. They fit naturally into existing medical workflows, reduce cognitive load for doctors and eliminate ambiguity at every step.
Whether you’re looking to build an internal system for your clinic or develop a SaaS product for the broader healthcare market, the fundamentals remain the same for everyone. Clarity, reliability, seamless integration!
P.s. And if you want to get it right from the start, working with a development team that understands both the technical side and the specifics of healthcare, is a major advantage. With hands-on experience in this domain, ein-des-ein can help you design and deliver an application that is not only functional but truly effective in real clinical environments!



